The Pan American Health Organization (PAHO) has launched a new tool aimed at helping Caribbean and other countries across the Americas sharply reduce heart attacks and strokes—two of the region’s leading causes of death. Known as the HEARTS Quality Framework, the practical guide was published in The Lancet Regional Health – Americas and is designed for immediate use within primary health care systems.
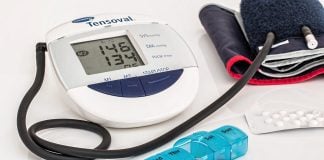
Cardiovascular disease claims more than 2.2 million lives each year in the Americas, many of them among working-age adults. In the Caribbean, where noncommunicable diseases (NCDs) such as hypertension, diabetes and heart disease already place heavy strain on public health systems, the burden is particularly acute. Nearly four in 10 adults in the region live with high blood pressure, often without knowing it. Despite the availability of low-cost, effective treatment, only one in three people with hypertension has their condition under control.
“Hypertension remains the world’s deadliest health threat, but also one of the most manageable,” said Dr. Jarbas Barbosa, Director of PAHO. He described the framework not as a theoretical policy, but as a proven guide already improving outcomes in community clinics across the region. “If countries adopt and scale it up, we can prevent millions of heart attacks and strokes over the next decade,” he said.
A blueprint built for primary care
The HEARTS Quality Framework draws directly from real-world experience in clinics that have successfully improved blood pressure control. It targets common gaps that affect Caribbean health systems, including unreliable blood pressure measurements due to outdated equipment, inconsistent access to essential medicines, unnecessary monthly clinic visits for prescription renewals, and limited use of team-based care.
Among its key recommendations are the use of validated automated blood pressure monitors; pooled procurement to ensure a steady supply of affordable, high-quality medicines; multi-month prescriptions to reduce patient burden; and expanded roles for trained nurses to adjust medication doses. The framework also introduces simple monitoring tools that allow clinics to track outcomes and continuously improve care.
HEARTS in the Americas is the largest global adaptation of the World Health Organization’s HEARTS initiative. It is now active in 33 countries, reaching nearly 10,000 primary care facilities and managing care for more than six million people through standardized treatment protocols. Where the approach is fully implemented, six in 10 patients achieve blood pressure control—almost double the regional average.
Implications for the Caribbean
For Caribbean countries grappling with limited resources and rising NCD-related costs, the framework offers a pathway to stronger, more efficient primary health care. PAHO officials note that effective hypertension control supports the region’s broader health and development goals by keeping adults healthier for longer and reducing avoidable hospitalizations.
The framework is closely aligned with the 80-80-80 target for blood pressure control: 80% of people with hypertension diagnosed, 80% of those diagnosed treated, and 80% of those treated achieving control. According to Dr. Pedro Orduñez, PAHO Senior Advisor for Cardiovascular Disease, meeting this target could prevent more than 400,000 deaths and 2.4 million hospitalizations across the Americas by 2030.
“We urge ministries of health, policymakers and health-care providers to adopt the HEARTS Quality Framework,” said Dr. Anselm Hennis, PAHO’s Director of Noncommunicable Diseases and Mental Health. “By committing to this model, we can deliver better care for NCDs, save lives, and strengthen primary health care systems—especially in small island and middle-income settings.”
Proven results across the region
Countries that have adopted the HEARTS approach are already reporting measurable gains. In Trinidad and Tobago, along with communities in Colombia and Mexico, clinics have seen sustained improvements in blood pressure control. In Cuba’s Matanzas province, control rates increased from 36% to 58% in just one year, while Chile reported a rise from 37% to 65%.
In the Dominican Republic, HEARTS has become a government priority, providing free hypertension treatment to millions. El Salvador expanded the approach nationwide, achieving control rates nearing 70%, and Mexico has begun implementing the program across its primary care network. Economic analyses show the model can pay for itself in under two years by preventing costly cardiac events.
“These results show that hypertension control at scale is possible,” said Dr. Esteban Londoño, PAHO international consultant and lead author. “Primary health care built on standardized pathways, reliable medicines and team-based care can have a life-saving impact for millions—including across the Caribbean.”
As Caribbean health leaders continue to confront the growing toll of NCDs, PAHO’s new framework offers a tested, adaptable roadmap to tackle one of the region’s most persistent—and preventable—health threats.