Cervical cancer remains one of the most preventable forms of cancer, yet it continues to claim the lives of women every year — largely because too many are diagnosed too late.
January, recognized as Cervical Health Awareness Month, shines a spotlight on a disease that medical experts say should rarely reach advanced stages in countries with access to basic screening. The disconnect, they warn, lies not in medical capability but in delayed testing, limited access to care, and persistent misinformation.
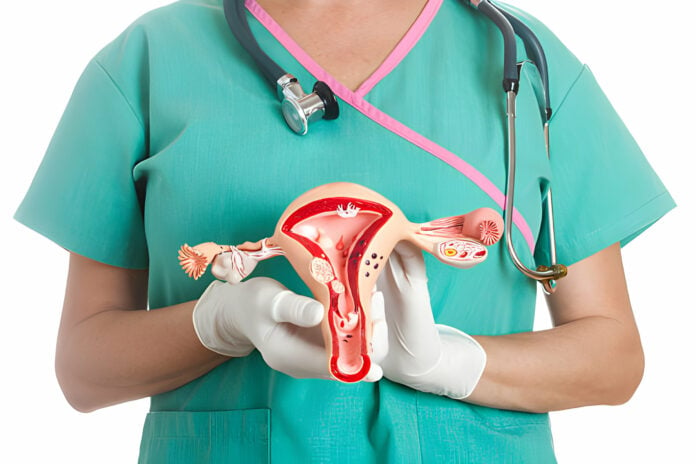
The vast majority of cervical cancer cases are caused by persistent infection with the human papillomavirus (HPV), a common sexually transmitted virus. While most HPV infections clear naturally, certain high-risk strains can remain in the body for years, gradually causing abnormal changes in cervical cells. Left undetected, those changes can progress to cancer.
What makes cervical cancer particularly dangerous is that early stages usually produce no symptoms. By the time warning signs such as abnormal bleeding or pelvic pain appear, the disease may already be advanced. This is why doctors stress that screening — not symptoms — is the primary defense.
Routine Pap smears and HPV tests can detect precancerous changes long before cancer develops. When abnormalities are caught early, treatment is often straightforward and highly effective. Health authorities have repeatedly emphasized that regular screening can prevent the majority of cervical cancer cases.
Despite this, screening rates remain uneven. Studies consistently show that women of African descent, including Caribbean and diaspora populations, are more likely to be diagnosed at later stages and to experience higher mortality rates. Barriers include cost, lack of insurance, limited clinic access, fear of the exam, and cultural stigma surrounding gynecological care.
Vaccination offers another powerful layer of protection. The HPV vaccine guards against the strains most commonly linked to cervical cancer and is most effective when administered before exposure to the virus. While vaccination programs have expanded globally, uptake remains inconsistent, particularly in communities where misinformation and access challenges persist.
Public health advocates say reducing cervical cancer deaths requires more than awareness campaigns. It demands sustained investment in screening programs, education that normalizes preventive gynecological care, and policies that remove financial and logistical obstacles for women.
The reality, experts stress, is stark but hopeful: cervical cancer is not inevitable. With regular screening, vaccination, and timely follow-up care, most cases can be prevented entirely. Cervical Health Awareness Month serves as a reminder that prevention works — but only when women are able, informed, and empowered to access it.